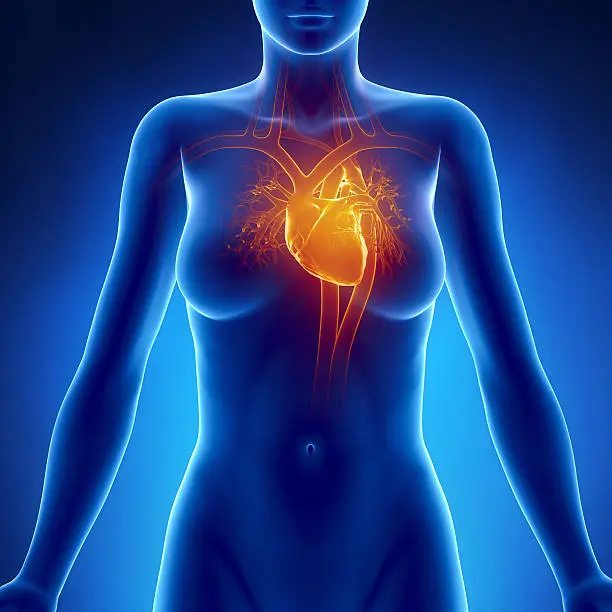
Causes Of Heart Attack In Women
Most heart attacks are indirectly caused by coronary artery disease (CAD) or Atherosclerosis, a condition in which fatty deposits (plaque) build up on the walls of an artery. This narrows the arteries and restricts blood flow to the muscle of the heart. A heart attack is usually triggered by a tear or rupture of the plaque, which leads to the formation of a blood clot that blocks the blood flow in the artery. Spasm of the artery can also contribute to the blockage.