An Atrial Septal Defect is a common congenital heart condition that can remain undetected for years. While some individuals may not experience noticeable symptoms early on, an untreated atrial septal defect can lead to serious complications, including pulmonary hypertension, which significantly affects heart and lung function.
Understanding the risks, symptoms, and long-term effects of an atrial septal defect is essential for early diagnosis and effective management. Regular monitoring and timely treatment can help prevent irreversible damage and improve long-term heart health.
What Is an Atrial Septal Defect?
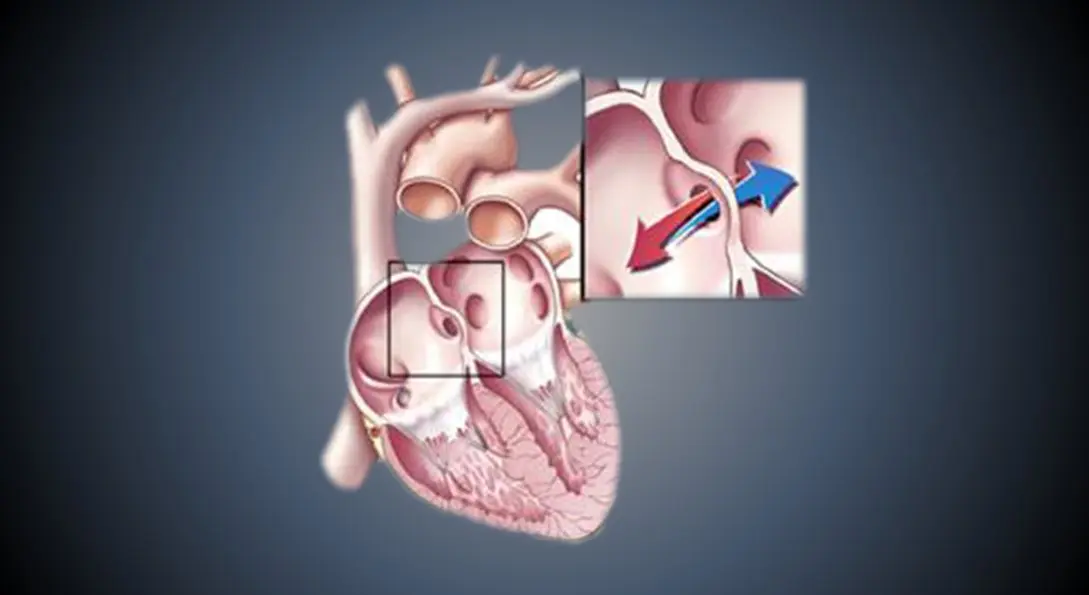
An Atrial Septal Defect is a hole in the septum, the wall that separates the heart’s two upper chambers (atria). This opening allows oxygen-rich blood from the left atrium to flow into the right atrium instead of circulating properly through the body.
This abnormal blood flow is known as a left-to-right shunt. Over time, it increases the volume of blood flowing to the lungs, placing extra strain on both the lungs and the right side of the heart.
While small defects may not cause immediate problems, larger or untreated atrial septal defects can lead to serious cardiovascular complications.
How an Atrial Septal Defect Leads to Pulmonary Hypertension
One of the most important complications of an atrial septal defect is the development of pulmonary hypertension (PH).
The Underlying Mechanism
- Blood flows abnormally from the left atrium to the right atrium
- This increases blood flow to the lungs
- The lungs experience continuous overcirculation
- Increased flow causes shear stress on pulmonary vessels
- Over time, this leads to vascular remodeling
- Pulmonary artery pressure gradually increases
As a result, patients may develop pulmonary arterial hypertension (PAH), a serious condition that can damage the heart and lungs.
Studies show that pulmonary hypertension develops in approximately 6% to 35% of patients with untreated large atrial septal defects, highlighting the importance of early monitoring.
Symptoms of Atrial Septal Defect
An atrial septal defect may not cause symptoms in its early stages. However, as the condition progresses, patients may begin to notice signs that should not be ignored.
Common Symptoms Include:
- Shortness of breath (dyspnea), especially during activity
- Fatigue or persistent tiredness
- Heart murmur, often detected during routine examination
- Right-sided heart failure in advanced cases
These symptoms may develop gradually and are often mistaken for less serious conditions, which can delay diagnosis.
Why Symptoms Should Not Be Ignored
One of the biggest challenges with an atrial septal defect is that symptoms are often subtle or slow to appear. Many patients dismiss early warning signs such as fatigue or mild breathlessness.
However, delaying medical evaluation can allow the condition to progress to pulmonary hypertension or other complications. Once significant damage occurs, treatment options may become limited.
Early recognition of symptoms and timely consultation with a cardiologist can prevent long-term complications and improve outcomes.
Diagnosis of Atrial Septal Defect
Accurate diagnosis of an atrial septal defect is essential for proper management and prevention of complications.
Primary Diagnostic Tool
- Transthoracic Echocardiography (TTE) is the most commonly used test
- It provides detailed images of heart structure and blood flow
Additional Diagnostic Methods
- Agitated saline (bubble study) may be used to confirm the presence of a shunt
- Right heart cardiac catheterization helps measure pressure in the heart and lungs
These tests help determine the size of the defect, the severity of blood flow abnormalities, and the presence of pulmonary hypertension.
Management and Treatment of Atrial Septal Defect
Treatment of an atrial septal defect depends on the size of the defect, symptoms, and pulmonary vascular resistance (PVR).
Role of Right Heart Catheterization
Before deciding on treatment, a right heart catheterization is often performed to assess:
- Pulmonary artery pressure
- Pulmonary vascular resistance (PVR)
This information is critical in determining whether the defect can be safely closed.
When Closure Is Recommended
Closure of an atrial septal defect is typically recommended when:
- Pulmonary vascular resistance (PVR) is less than 5 Wood units
- The heart can tolerate the closure
Closing the defect helps normalize blood flow and prevents further complications.
“Treat and Repair” Approach
For patients with elevated pulmonary pressure:
- If PVR is greater than 5 Wood units, immediate closure may not be safe
- Patients are treated with pulmonary arterial hypertension (PAH) medications
- Once pressures are reduced, closure may be considered
This strategy improves safety and treatment outcomes.
When Closure Is Contraindicated
In advanced cases, patients may develop Eisenmenger syndrome, where the blood flow reverses (right-to-left shunt).
In this situation:
- Closing the atrial septal defect is not recommended
- The defect acts as a pressure relief (“pop-off”) valve
Closing it can worsen the condition and lead to severe complications.
Importance of Regular Monitoring
A key part of managing an atrial septal defect is ongoing monitoring through echocardiograms.
Regular follow-up helps:
- Track changes in heart structure
- Monitor blood flow patterns
- Detect early signs of pulmonary hypertension
- Guide timely intervention
Key Takeaway
Atrial Septal Defect must be monitored regularly with echocardiograms.
Even if symptoms are mild or absent, consistent monitoring is essential to prevent long-term complications.
Long-Term Risks of Untreated Atrial Septal Defect
If left untreated, an atrial septal defect can lead to serious health issues, including:
- Pulmonary hypertension
- Right-sided heart failure
- Arrhythmias (irregular heart rhythms)
- Stroke
- Eisenmenger syndrome
These complications can significantly impact quality of life and may become life-threatening.
When Should You See a Cardiologist?
You should consult a cardiologist if you experience:
- Shortness of breath during routine activities
- Unexplained fatigue
- Heart murmur
- Symptoms that worsen over time
- Known or suspected congenital heart condition
Early evaluation allows for accurate diagnosis and timely treatment.
Preventing Complications of Atrial Septal Defect
While an atrial septal defect itself cannot always be prevented, its complications can be minimized with proper care.
Key Preventive Measures:
- Regular cardiac checkups
- Routine echocardiograms
- Early treatment when recommended
- Monitoring for symptoms
- Following medical advice closely
Timely intervention can significantly reduce the risk of pulmonary hypertension and other complications.
Final Thoughts
An Atrial Septal Defect may appear harmless in its early stages, but it can lead to serious complications if left untreated. The development of pulmonary hypertension is one of the most significant risks associated with this condition.
Recognizing symptoms, undergoing regular monitoring, and following appropriate treatment plans are essential steps in managing this condition effectively.
Most importantly, symptoms such as shortness of breath and fatigue should never be ignored. Early diagnosis and intervention can help prevent long-term damage and improve overall heart health.

